Baylor Scott & White The Heart Hospital – Plano has the largest cardiothoracic robotic surgery program in Texas—and has recently achieved what few hospitals worldwide have: 1,000 cardiothoracic procedures using minimally invasive robotic surgery.
A talented football and baseball player, Camden Thrailkill was just 15 years old when he was diagnosed with mitral insufficiency. The mitral valve in his heart didn’t close properly when it pumped out blood. In essence, his heart wasn’t working properly. To save his life he required a mitral valve replacement—open heart surgery. An incision anywhere from six to 10 inches would be made along the middle of his chest and his breastbone sawed open to expose the heart. Following the surgery he would spend at least one day in the ICU, seven to nine days in the hospital and another six to eight weeks in recovery. His breastbone—wired back together—would never fully recover. It would be permanently damaged, forever fragile and at constant risk of breaking and crushing his heart. He would never play football again. His career as an athlete should have been over before it had even begun.
Thanks to robotic surgery, Camden had a very different outcome. Following robotic-assisted surgery at Baylor Scott & White The Heart Hospital – Plano in October 2016, Camden spent just one night in the hospital, missed only three weeks of school and started working out again within a month. Today, just six months after his surgery, he’s already back on the playing field.
Read more: Baylor Scott & White The Heart Hospital – Plano opens new North Tower
It’s a story Mark Valentine, president of Baylor Scott & White The Heart Hospital – Plano, relays with pride when we meet to discuss the future of surgery—robotics—happening now at Baylor Scott & White The Heart Hospital – Plano.
“Robotic surgery is a different technique that’s less invasive. It allows the surgeon to do a better job and patients to recover more quickly,” explains Dr. G. Kimble Jett, Medical Director of Thoracic Surgery at Baylor Scott & White The Heart Hospital – Plano.
I meet with Dr. Jett at 7 a.m. on a Tuesday. “Tuesdays are my robot days,” he says with a smile as we dress in scrubs for the OR. “My patients will go home Wednesday or Thursday, a lot go back to work the next week,” he adds.
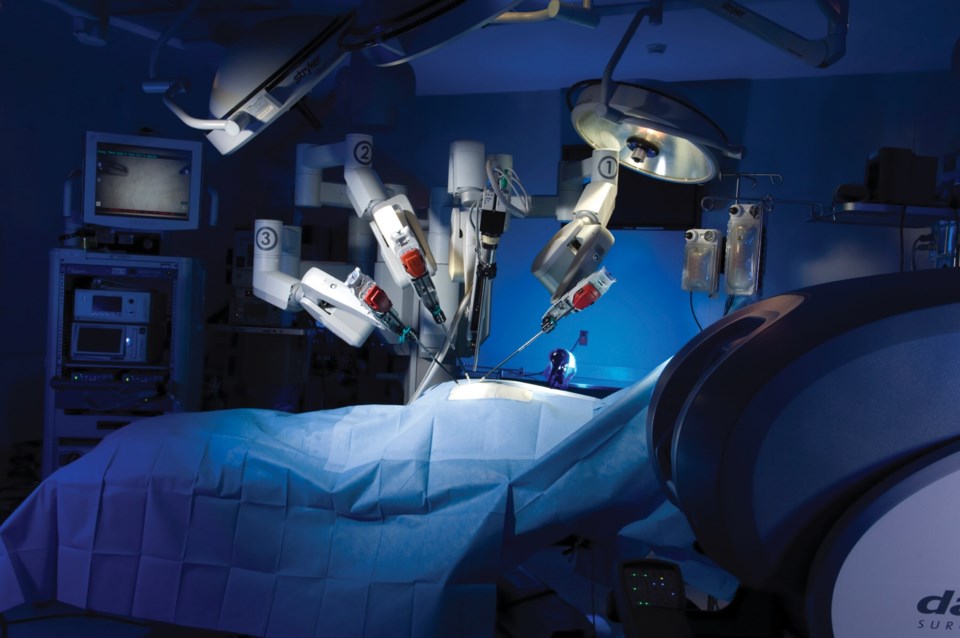
The da Vinci robot is decidedly underwhelming. It looks just like any other piece of medical equipment: white, metallic, clean. When I see it in action (via a video since I’m not allowed into an actual surgery), I’m amazed.
In order to perform a lobectomy—which normally requires a 10-inch incision along the side of the chest, followed by spreading of the ribs—Dr. Jett inserts four ports which vary in size from the width of my pinky to the width of my index finger. It is through these ports that the camera and operating tools are inserted. A fifth port, called the assistant, is inserted below the lung and used as the exit point for any removed tissue. That’s it. “You end up with incisions the size of your fingernail,” Dr. Jett says.
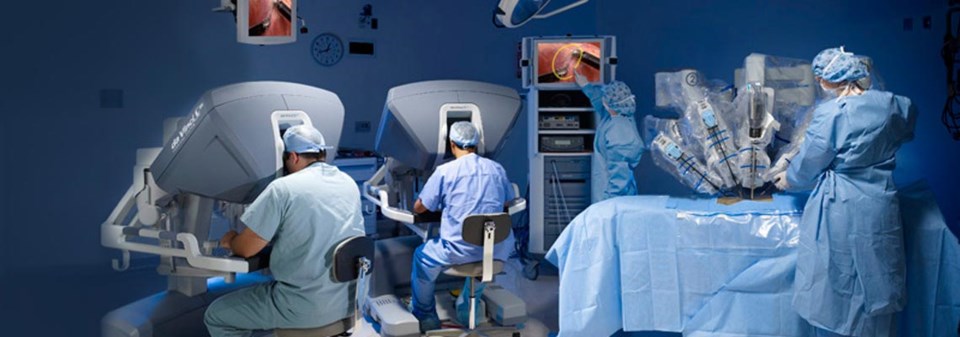
With the ports inserted, the robot is “docked” and Dr. Jett sits off to one side. With his head pressed against the console he’s able to see inside the patient—via high-definition, real-time images from cameras attached to one of the robotic arms. His hands and feet operate the tools.
“There are a lot of advantages of the robot. First of all you have improved vision; it magnifies it ten times. It’s a three dimensional camera; the da Vinci robot camera has two cameras together—a right eye and a left eye. You’ve got little instruments that move in seven different ways, so it’s like you’ve got multiple hands in there but they’re more stable. It’s as steady as a rock, so you have perfect precision.”
Of course, surgery of any kind is not always straightforward. Sometimes a robotic surgery has to be converted to an open surgery. “In our first 300 cases we had to open 11 people, about 3 percent. Of those, only two were converted due to bleeding. In our next 300 it was two total,” he says. “You do have complications, you can have bleeding, you do have to open people. But the nice thing about the robot is that you can do it in a controlled fashion and it occurs less frequently.”
The surgery takes about two hours; the same length of time as a traditional surgery. But recovery is much faster, and complications are dramatically lower, about 14 percent compared to 45 percent for open surgery.
Read more: Baylor Scott and White Sports Therapy & Research opens at The Star
So why are the majority of surgeons still doing open surgery?
“Robotic surgery has huge benefits for the patient, but not for the surgeon,” Dr. Jett explains. “It’s hard,” he adds. Robotic surgery requires retraining, hours dedicated to learning a new skill.
“As people see the results I think more surgeons will start doing it. As a consumer, as a patient, you really should Google and see what’s available so that when you do talk to your specialist you can make an educated decision.”
While many surgeons do need to retrain, they don’t need to worry that their job will be replaced by robots. “I think the surgeon will always control the robot; there won’t be some magic button you press,” he laughs as he tugs off a surgeon’s cap patterned with cowboy boots.
“One thing that may develop is remote robotic surgery. They’ve tried to do it overseas, there’s a little bit of a delay, which is a little cumbersome, but as they improve that you may be able to do robotic surgery on someone out, you know, in East Texas. You could have a team that puts all the ports in and the operating surgeon can be offsite to do the surgery.”
In the future of surgery, five hands—three of them robotic—are better than two.